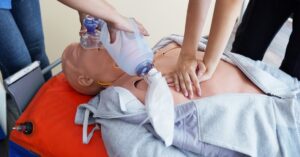
Understanding the various codes you can implement is important when working in a hospital. Listening closely to everything around you is key. New medical professionals must act calm and focused under pressure, even though everything around them seems accelerated. You must do the right thing when you notice your patient is in cardiac arrest—such as knowing one of many ways to call a code blue in a hospital. Learn more below.
What Is a Code Blue?
While you may call numerous codes when you work in a hospital, a code blue is likely one you’ll hear most often. You call a code blue when your patient experiences unexpected respiratory or cardiac arrest or another respiratory or cardiac emergency. These events require immediate medical attention and draw the focus of everyone in the hospital to the problem. At that point, it’s all hands on deck. While a designated “code team” responds to emergencies like this, a nurse will need to step away from whatever they’re doing and intervene if they’re close by.
Why Is It Important?
Ensuring everyone has the proper training for this call is important because several people will be getting involved. Code blues happen daily in hospitals for a variety of reasons, so this training can save a life. Therefore, we’ll show you one way you can properly call a code blue in a hospital below but know different hospitals may have different procedures.
Recognize When a Situation Calls for It
The first thing you need to do before calling a code blue is to recognize when you need to call one. You must know when your patient is decompensating acutely, so you can activate the emergency response at the right time—this is when you call the code blue.
You can begin CPR and call a coding team if you notice your patient isn’t responding to you, has no pulse, or isn’t breathing. These rapid response units are spectacular when needed but a waste of resources when they aren’t.
The first thing you need to do when determining whether to call the coding team is to keep your eyes on the patient whenever a monitor alarm goes off. One of the easiest ways to verify this is to know when their vitals are rapidly declining. Figuring this out is simple but gruesome: Do they look alive? It might not seem like it, but a person actively experiencing cardiac arrest almost looks deceased. You can expect to see the following:
– They will have greyish skin.
– They’ll feel cold and clammy to the touch.
– Their eyes will be glassy or rolled back in their head.
– They’ll release their bowels.
– Finally—and this is the most obvious—there will be no pulse.
Always Prepare
The first thing you need to do to prepare for a potential code blue is to know the patient’s code status. The code status is the type of treatment a person receives if they stop breathing or their heart stops beating. Some patients have a strict Do Not Resuscitate code that tells you not to attempt to renew them should they go into cardiac arrest. Accidentally resuscitating a patient who specifically said they didn’t want it could lead to a lawsuit.
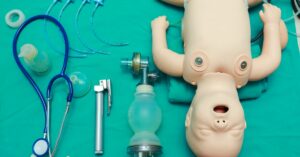
Make sure your suction is fully functional and set up properly. It may surprise you how often medical professionals do not test or set them at the ready. You want to prepare when the time comes. You need suction to help you with resuscitation in most cases. Make sure your oxygen is also fully functioning. Your patient’s oxygen mask must be accessible if they have one. You’ll also want to put an anbu-bag nearby and locate the CPR lever on all beds. These levers are usually bright red and almost always labeled “CPR.” Finally, know where your code button is in the room, the hallways, and the patient’s bathroom.
How To Respond Effectively
Now that you’re ready, it’s time to figure out how to respond. Have confidence that you can intervene because you’ll need it. First, push the code button to get help to the room as quickly as possible. You can even yell for the crash cart. The code button alerts everyone that should be in the room to come quickly. You’ll have a whole team with you in minutes, from the pharmacy to nursing and doctors’ practitioners. Don’t be shy if you can’t get to the code button quickly enough, shout that you have a code blue in your room.
You’ll also want to ensure your patient can receive CPR. Either lay them flat on the bed or the floor immediately. Since you know where the lever is on all your beds, press it and get the patient flat on their back.
After that, begin your compressions. You have the relevant certifications, so you know what to do. Press hard and fast. You’re trying to save a life, and quality chest compressions will help, even if the patient is sore and has a few broken ribs later. It’s better that they feel sore the next day than not have a next day at all. Focus on your form, and if you need to sing a song under your breath at 110 beats per minute, do so.
You will likely have your coding team in the room by this time. The next thing you’ll want to do is get a backboard under the patient unless they are already on the floor. Make sure there are pads in place. Switching from floor to backboard might take a bit, depending on how long you’re compressing their chest.
Finally, since the entire team is on board, the best thing you can do is watch what’s happening if you’re a new or inexperienced nurse, no matter what the outcome. Learn what techniques and forms they’re using. You’ll learn many nuances, including the “pulse check” between resuscitation measures. Don’t hesitate to ask to switch places with someone on the code team. It’s easy to tire yourself out, and that’s why you have a team—they can help you when you need it. Take advantage of this and remain calm.
Nothing can help you more than a CPR class to learn more about resuscitating someone experiencing cardiac arrest. No matter who you are, learning these techniques is important. We host many in-person and online classes at CPR123. Check out our ACLS classes for healthcare providers if you need or want to brush up on your CPR training. We’ll teach you everything you need to know so you can be ready to assist in the event of a cardiac arrest.