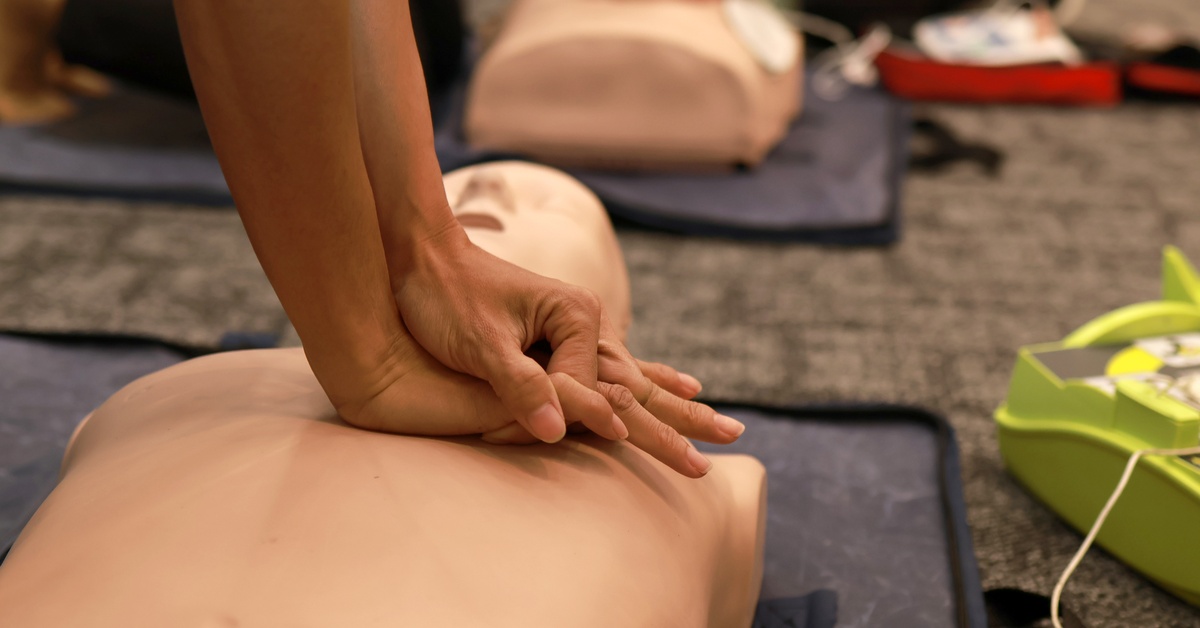
You see how instructors teach CPR today, and it can feel like that’s how it’s always been done. It hasn’t. The systems behind modern CPR grew through decades of trial, research, and real-world emergencies.
A look at the history of basic life support strategies shows how lifesaving actions changed as medicine learned what actually keeps people alive. Whether you’re brand new or you’ve trained for years, knowing where these practices came from gives you better context for why they matter now.
Early Attempts at Reviving the Unconscious
Long before CPR had a name, people tried to bring others back using whatever methods made sense at the time. Some early approaches included manual stimulation, forceful breathing attempts, or physical movement to restart breathing.
These actions lacked scientific backing, but they shared one goal. People wanted to restore breathing and circulation fast. Even without modern knowledge, responders understood that delay often led to death.
These early methods varied widely across regions and cultures. Some relied on warming the body or repositioning the person to improve airflow. Others focused on aggressive physical techniques that later proved harmful. While many of these actions missed the mark, they highlighted a consistent understanding. Intervention mattered, even when science wasn’t clear yet.
The Shift Toward Airway and Breathing Focus
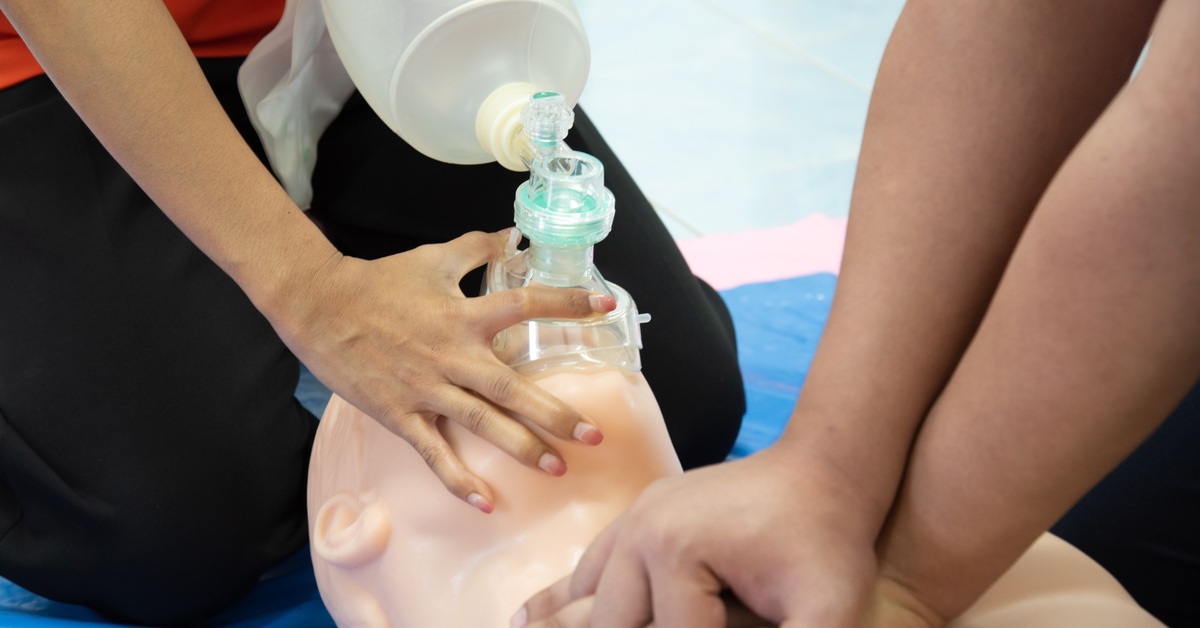
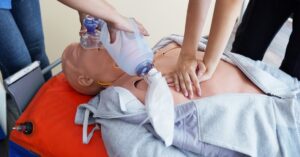
As medical research advanced, providers began to understand the role of oxygen. This led to structured attempts to open the airway and support breathing. Mouth-to-mouth ventilation gained attention during the mid-20th century after studies showed it moved enough oxygen to sustain life. This shift marked an essential step toward standardized care. Breathing support became a defined action instead of a guess.
This period also introduced clearer teaching methods. Providers learned how head positioning affected airflow and how improper techniques reduced effectiveness. Training emphasized consistency so responders could act quickly without hesitation. These developments laid the groundwork for teaching lifesaving skills in a repeatable way.
Chest Compressions Change Everything
The discovery that external chest compressions could circulate blood reshaped emergency response. Researchers demonstrated that rhythmic pressure on the chest could maintain blood flow to the brain and heart.
This finding replaced older, ineffective circulation methods. Once compressions proved reliable, they became a foundation of care. Modern CPR wouldn’t exist without this breakthrough.
Early compression techniques weren’t perfect. Rates and depth varied until studies clarified what produced adequate circulation. Over time, data confirmed that strong, consistent compressions improved survival. These findings reinforced the idea that circulation mattered as much as breathing during cardiac arrest.
Standardization Through Medical Organizations
As evidence grew, medical organizations stepped in to create consistency. Guidelines unified how providers approached cardiac arrest. These standards helped remove guesswork and reduce variation between responders. Leaders aligned training programs around the same sequence of actions. This consistency improved survival rates across different settings.
Standardization also supported accountability. Instructors could measure performance against clear benchmarks. Healthcare systems gained confidence that trained providers shared the same foundation. This alignment strengthened teamwork during emergencies when coordination mattered most.
The Role of Training and Repetition
Basic life support skills rely on muscle memory. Early programs showed that repetition improved response speed and accuracy. Providers who received regular training performed better under stress. This understanding shaped certification models that we still use today. Structured practice became just as important as knowledge.
Repeated hands-on practice helped reduce hesitation during real emergencies. Providers learned how it felt to deliver proper compressions and manage airways correctly. This familiarity improved confidence when seconds mattered. Training also reinforced teamwork, enabling responders to anticipate one another’s actions and communicate clearly under pressure.
Technology Influences Modern Techniques
Defibrillators changed how responders approached sudden cardiac arrest. Portable AEDs allow for faster intervention outside hospitals. Guidelines evolved to integrate these devices smoothly into care. Technology didn’t replace basic skills. It strengthened them because responders still need solid fundamentals to use new tools correctly.
As technology advanced, training adapted alongside it. AED prompts guided users, but correct pad placement and timing still depended on human action. Providers learned to balance device use with manual skills. This combination improved outcomes when equipment was available and reinforced fundamentals when it wasn’t.
Expanding Beyond Healthcare Settings

Basic life support stopped being limited to hospitals. Schools, workplaces, and public spaces adopted these life-saving training programs. This expansion recognized that emergencies don’t wait for professionals. Teaching lay responders increased early intervention rates. Faster action often meant better outcomes.
Public training programs focused on simple, repeatable actions anyone could perform. These courses emphasized recognizing cardiac arrest, calling for help, and starting care immediately.
Communities with higher training participation reported quicker response times before EMS arrival. Early action helped preserve brain function and circulation, giving advanced care a stronger starting point when professionals took over.
Continuous Updates Based on Research
Medical knowledge doesn’t stand still. Ongoing studies continue to refine compression depth, rate, and ventilation timing. Guidelines adjust when evidence shows better results. This cycle keeps care current and effective. Providers benefit when training reflects what works right now.
These updates also influence how often providers practice their skills. Research shows that performance declines without regular review. Training models evolved to emphasize refreshers and hands-on evaluation. Staying current protects both the provider and the patient.
Why History Still Matters Today
Understanding how these strategies evolved explains why steps happen in a specific order. Each action exists because research has proven its value. Skipping fundamentals weakens the entire response.
History also clarifies why shortcuts fail under pressure. Proven sequences reduce confusion when stress is high and time is limited. Providers who understand the reasoning behind each step respond with greater confidence and consistency. This perspective strengthens decision-making during emergencies and reinforces respect for established protocols that protect patient outcomes.
Bringing It All Together for Modern Training
Modern courses reflect decades of progress. They focus on airway control, circulation, and early defibrillation because those steps save lives. If you’re maintaining your skills or updating credentials, enrolling in a BLS renewal course keeps your approach aligned with current standards. A Look at the History of Basic Life Support Strategies shows that staying current isn’t optional. It’s essential for an effective response when seconds matter.